Arthrosis
Other specialties
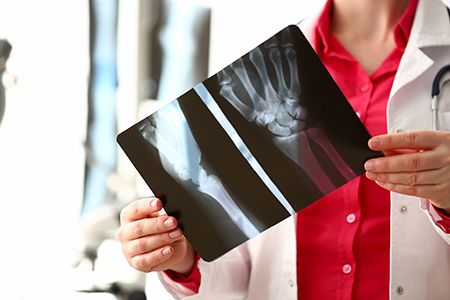
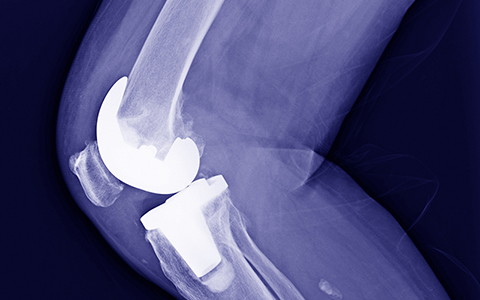
The degenerative pathology of all the joints in the body produces pain, disability and loss of mobility. We have various techniques to try to reduce the effects such as hyaluronic acid, plateletrich plasma (PRP), infiltrations with corticoids and even, in the most advanced processes, the alternative with surgery that goes from platelet osteotomies to a, the replacement of the joint with a prosthesis, always offering an individualized treatment.
Osteoarthritis is a rheumatic pathology that damages the articular cartilage. The joints are the components of the skeleton that allow us to move and therefore our functional autonomy and are formed by the union of two bones through the joint capsule. Inside them there is generally a fluid called synovial fluid that is produced by the synovial membrane. The bone ends that join to form the joint are covered by articular cartilage.
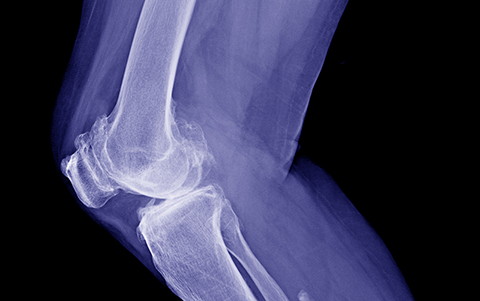
When this joint cartilage is injured, pain, stiffness, and disability occur. Osteoarthritis is usually located in the cervical and lumbar spine, some joints of the shoulder and fingers, the hip, the knee, and the joint at the beginning of the big toe.
It is important to differentiate it from arthritis, as in arthritis it is inflammation that causes the disease and in osteoarthritis it is “wear and tear”. These are two diseases that cause pain, sometimes swelling and stiffness, but in osteoarthritis the pain is mechanical (that is, it is triggered by movement and improves with rest).
This rheumatic disease is not hereditary, but it does have a genetic risk component which, together with other factors, can make it appear more easily in subjects who have a family history. It is important to know this and also to know that risk factors such as obesity, lack of physical exercise or alterations in posture influence the development of the disease and modify them is within the reach of the patient himself both to prevent or delay symptoms and to encourage treatment.